If you attend yearly wellness evaluations with your regular health care provider, you have probably heard us talk about when you are due for a colonoscopy. So what is a colonoscopy, and why are we talking about it?
A colonoscopy is one of several tests used to identify precancerous changes, early cancerous lesions, or cancer of the colon.
We call cancers of the colon “Colorectal Cancer.” Colorectal cancer is the second leading cause of cancer death for both men and women (preceded only by lung cancer). 52,980 people in the US are expected to die of colorectal cancer in 2021. It is most frequently diagnosed in persons age 65-74. However, 10.5% of new colorectal cancer cases occur in persons younger than 50 years old, and cases of this cancer have increased almost 15% from 2000-2002 to 2014-2016 in persons age 40-49. Because of this change, the US Preventative Task Force recently changed its recommendation for screening colonoscopies to begin at age 45. However, most insurance guidelines still follow the previous guidance of age 50, so this test isn’t covered as a screening test before age 50 yet. (This is different if you have a family history! For example, suppose someone in your immediate family, like a parent or sibling, had colon cancer. In that case, it is recommended you have a colonoscopy when you are ten years younger than your family member was when they were diagnosed, or age 50, whichever comes first.)
Colon cancer often has no symptoms early on when it is easiest to treat. When it does cause symptoms, it can cause stomach pain, a change in bowel movements, blood in bowel movements, and feeling tired or weak. The goal is to find precancerous changes before they progress and cause any symptoms or damage.
So what makes a colonoscopy such a great cancer-reducing tool?
The primary goal of colorectal cancer screening is to prevent deaths from colorectal cancer. Screening tests can help identify cancers at an early and potentially curable stage. Screening can also prevent cancer by identifying and treating abnormal precancerous growths (polyps) that can be removed before they become cancer. So you can be screened and treated for pre-colon cancer lesions, all during the same test.
The Background:
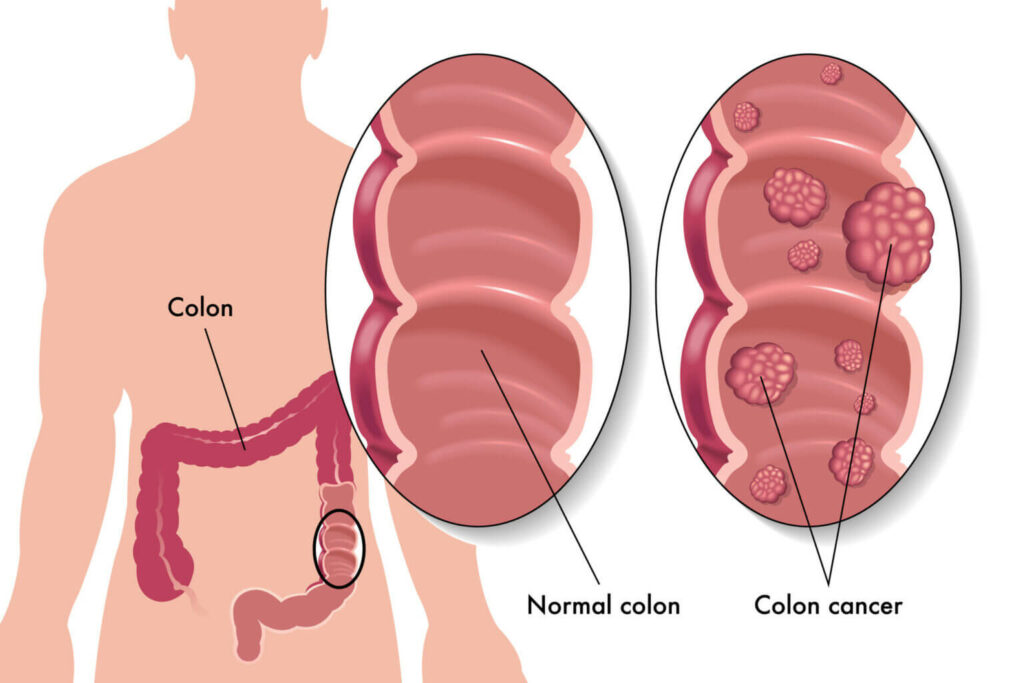
Most colorectal cancers develop from precancerous polyps. Polyps are growths that form in the lining of the colon. These polyps can develop into cancer over time, but this progression takes at least ten years in most people.
So during a colonoscopy, if a polyp is found, it is removed to try to prevent it from becoming more serious. Regular screening with colonoscopies for and removing polyps reduces your risk of developing colorectal cancer by up to 90%! Similarly, if a cancer is found, it may be treated, hopefully at an earlier stage than it would have been found otherwise. Early detection of cancers already presents in the colon increases the chance of successful treatment and decreases the chance of dying due to cancer.
So how do we get ready for a colonoscopy, and how does it work?
The Prep:
Colonoscopy requires that you prepare by cleaning out your entire colon so the provider can see the inside of your colon well. Essentially, they are looking through a small camera to look for changes in the intestine wall lining. So the colon wall needs to be clean for them to see.
This clean-out usually involves drinking a laxative liquid preparation that causes temporary diarrhea. This is by far the worst part of the colonoscopy experience. It is also a reason that many people avoid having a colonoscopy. Avoiding a colonoscopy, for this reason, is foolish as progressive colon cancer will cause far more symptoms than “temporary diarrhea.”

The Procedure:
Once prepped, you will go to your scheduled appointment at the “Colonoscopy Center” we sometimes refer to as the “GI Lab,” short for Gastroenterology Lab. There you will be given a mild sedative drug, or some providers use a more potent anesthetic agent that puts you to sleep. This might be the best part of the colonoscopy, the short but powerful “colonoscopy nap.”
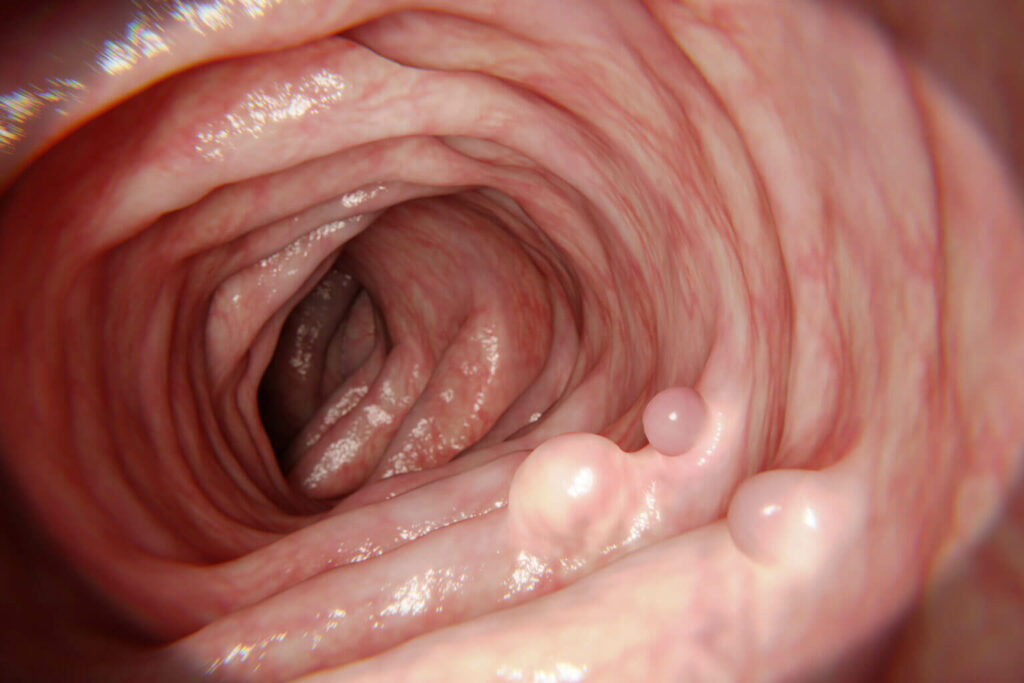
Once you are sedated, a thin, flexible, lighted tube is inserted through the anus and used to directly inspect the lining of the rectum and the entire colon. Biopsies (samples of tissue) may be taken during the procedure. Polyps and some cancers can be removed during this procedure. The whole process usually takes less than 30 minutes. You are given the news of your colonoscopy immediately, but you will need to wait for the pathology results for several days if you had removed polyps during the procedure. Pathology results help determine if additional treatments are required and how many years you can wait before your next colonoscopy.
You can rest and recover from the sedation and must have someone to drive you home and stay with you for several hours as you fully recover from the sedation. After that, you can typically resume life as usual.
Isn’t there an easier way?
There are several other screening tests we use to look for signs of colon cancer. However, none of them are as effective as a colonoscopy. Colonoscopy is the most sensitive of the available tests; it detects most small polyps and almost all large polyps and cancers and substantially lowers the risk of developing and dying from colorectal cancer.

Do we ever use colonoscopies for other reasons?
Yes! We use these useful diagnostic tools to identify other health problems also. For example, blood in your bowel movements, changes in your bowel habits, to evaluate for causes of anemia, or long term belly or rectal pain that we can not explain another way.
So, be as aggressive with your colon cancer screenings as you can! It is an almost entirely preventable cancer if we use colonoscopies effectively! Talk with your provider at your next visit about planning to have this vital screening completed.



